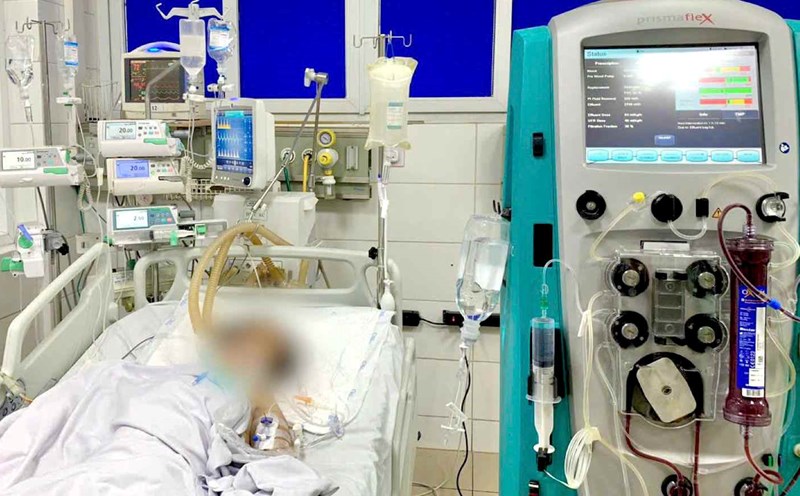
The Central Hospital for Tropical Diseases has just saved a 66-year-old male patient with a complicated soft tissue infection, post- cervical surgery, on the basis of many serious diseases and infections with resistant bacteria - a situation that often has a very bad prognosis if not treated intensively and coordinated with many specialties.
After falling from the 2nd floor, Mr. N.V.T in Tuyen Quang suffered a broken lumbar spine and had to undergo fixed surgery with a screening brace at a provincial hospital. However, the surgical incision was not immediately, and the pus was prolonged despite antibiotic use at many facilities. The patient was then removed from the bracelet, had the necrotizing facility filtered, and determined to have resistant bacteria. At the same time, the lungs suffered widespread damage, and the patient suffered from severe respiratory failure.
When transferred to the Central Hospital for Tropical Diseases, the patient was in critical condition: High fever, difficulty breathing, exhaustion. The lumbar surgical scar is more than 20cm long and over 10cm wide, revealing the spine, thick pus and widespread necrosis. Test results showed a CRP inflammation index of nearly 20 times normal, while CT images showed left lungs almost completely gone.
MSc. Dr. Dang Van Duong - Request and International Medical Examination Center - the person directly treating him - said: "The patient has diabetes, coronary artery stenosis, has had multiple surgeries, and is infected with resistant bacteria in many locations. This is an extremely difficult case due to the risk of multiple organ failure and widespread infection. Infection control requires a synchronous and accurate treatment process step by step.
The hospital held a consultation with the specialties of Surgery, Orthopedics and Neurology - Spine, underwent the first surgery to remove necrotizing tissue and install a negative pressure absorption (VAC) system to control pus, immediately promoting the wound. In parallel, antibiotics are used in the same way as antibiotics, combining respiratory support, nutrition and underlying disease control.
After 10 days, the patient's condition improved significantly: fever died, inflammation index decreased sharply, lungs recovered, wound was clean, and hat tissue developed well. The team performed a second surgery to re- place the screws and seal the surgical site.
Dr. Nguyen Thanh Tung - Deputy Head of the Department of Orthopedic Trauma and Spinal Neurology - said: "The surgery was smooth thanks to the wound foundation being well controlled, the patient recovered quickly after surgery".
After more than 35 days of treatment, the patient was completely stable, sat up on his own, practiced walking gently, had immediate surgical wounds and respiratory function returned to normal.
According to MSc. Duong, the case is a clear demonstration of the special role of the infectious disease hospital in handling complex post-operative infections. Without close coordination between infection and surgery, the risk of treatment failure will be huge.
The doctor recommends that patients after surgery - especially the elderly, with underlying diseases - if they see a surgical wound swollen, red, painful, or not immediately leakage after 5-7 days should go to a specialist hospital immediately for timely assessment and treatment, avoid complications of sepsis or have to remove the fixed equipment.