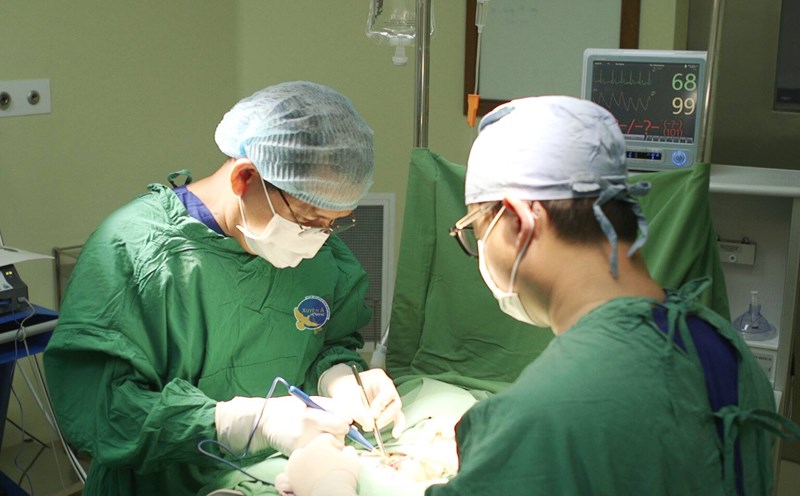
Abuse of thyroid cancer treatment, increasing health insurance costs
At the in-depth conference on thyroid cancer gathering many leading experts held on April 4 at Hong Ngoc Phuc - Truong Minh General Hospital, experts focused on updating new treatment methods and accurate damage assessment methods, contributing to unifying protocols, reducing overdoing treatment and improving effectiveness for patients.
According to Dr. Nguyen Trong Khoa - Deputy Director of the Department of Medical Examination and Treatment Management (Ministry of Health), Vietnam records about 6,100–6,200 new cases of thyroid cancer each year. This is the cancer with the best prognosis among many types of cancer.
However, there is currently a risk of overdiagnosis: Increased use of ultrasound, CT, MRI; Detection of many small tumors, slow progression; Many cases do not require immediate treatment.
Risk of over-treatment: High surgical rates, even with small tumors < 1 cm. This increases medical costs and systemic burden, affecting the patient's quality of life.
In actual implementation: Thyroid ultrasound is widely performed in periodic health check-ups; The rate of detecting thyroid nodules is high (19–68% of the population has thyroid nodules) but only 3–7% is cancer.
This leads to an increase in the number of unnecessary biopsies and surgeries, putting pressure on the upper-level hospital system, increasing HI costs.
In that context, the Ministry of Health clearly identifies that thyroid cancer is not a priority for reducing mortality, but a priority for reasonable management, avoiding medical abuse. We need to shift from: "Detected as much as possible" to "Detected correctly - treated correctly - managed appropriately".
The Ministry of Health will soon standardize protocols, build professional accreditation tools and apply AI to control treatment quality, reduce waste and risks for patients.
Need appropriate stratification and treatment
Dr. Nguyen Thi Phuong - Department of Nuclear Medicine - Central Military Hospital 108 said: To diagnose what kind of thyroid cancer is severe, doctors not only look at the name of the disease but must also rely on the risk stratification system.
Patients with papillary or differentiated thyroid cancer but classified as "high-risk" will need to apply more active and stronger treatment regimens than patients in the low-risk stratification group.
The concept of "healing" in thyroid cancer is often placed by doctors in quotation marks, because for papillomatic thyroid cancer or variants with good prognosis, the condition can still remain stable for a fairly long time even if the patient does not receive specific treatment but only applies active monitoring methods.
Even, according to Dr. Phuong, a study monitoring low-risk thyroid cancer patients lasting up to 20 years recorded very positive figures: only about 30% of cases showed signs of progression and the risk of death from the disease was only at 10-15%.
The above data shows that, despite being labeled "cancer", if properly stratified and treated appropriately, patients have complete hope of living healthy and stable for a long time.

According to Dr. Nguyen Trong Khoa, the issue of medical assessment is related to damage caused by thyroid cancer to serve as a basis for paying for economic insurance, social insurance and commercial life insurance, which are all related to each other.
Dr. Khoa emphasized that this is an issue that needs special attention, especially in the context of strategic transformation from "quick detection, early detection, multiple detection" to "correct detection, correct treatment".
To do that, it is necessary to continue to improve the legal corridor related to assessment, including the content of amending regulations on the rate of injury. The goal is to build a suitable and updated legal framework with the world, avoiding waste, avoiding excessive treatment, managing and treating according to current evidence.
Leaders of the Department of Medical Examination and Treatment Management also emphasized the requirement to access world scientific advances, from biomedicine, hormone therapy, radiation therapy to advances in diagnosis. Many new therapies such as immunotherapy and targeted therapy are developing, but access must be appropriate to resources, cannot be applied entirely but needs to be chosen based on actual conditions.
In addition to issuing regulations, it is necessary to strengthen implementation supervision. He suggested that experts develop a set of professional accreditation criteria to determine what is appropriate application, what is abuse, thereby responding to facilities and gradually improving the quality of diagnosis and treatment.
Another important content is professional support for lower levels, narrowing differences in access to diagnosis and treatment between facilities. It is necessary to gradually reduce the fluctuation range in applying professional guidance through training, distance medicine and updating new trends.
In the field of diagnosis and treatment planning, more technology can be applied, including AI, to completely reduce dependence on human factors, aiming to develop accurate treatment plans for each individual and appropriate monitoring in the later stages.