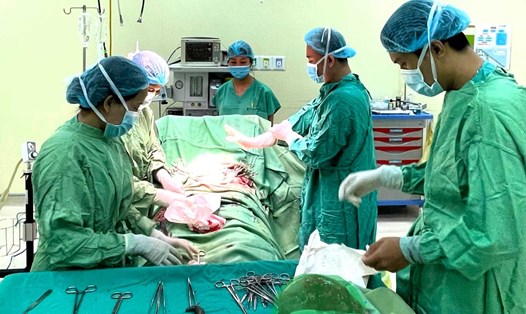
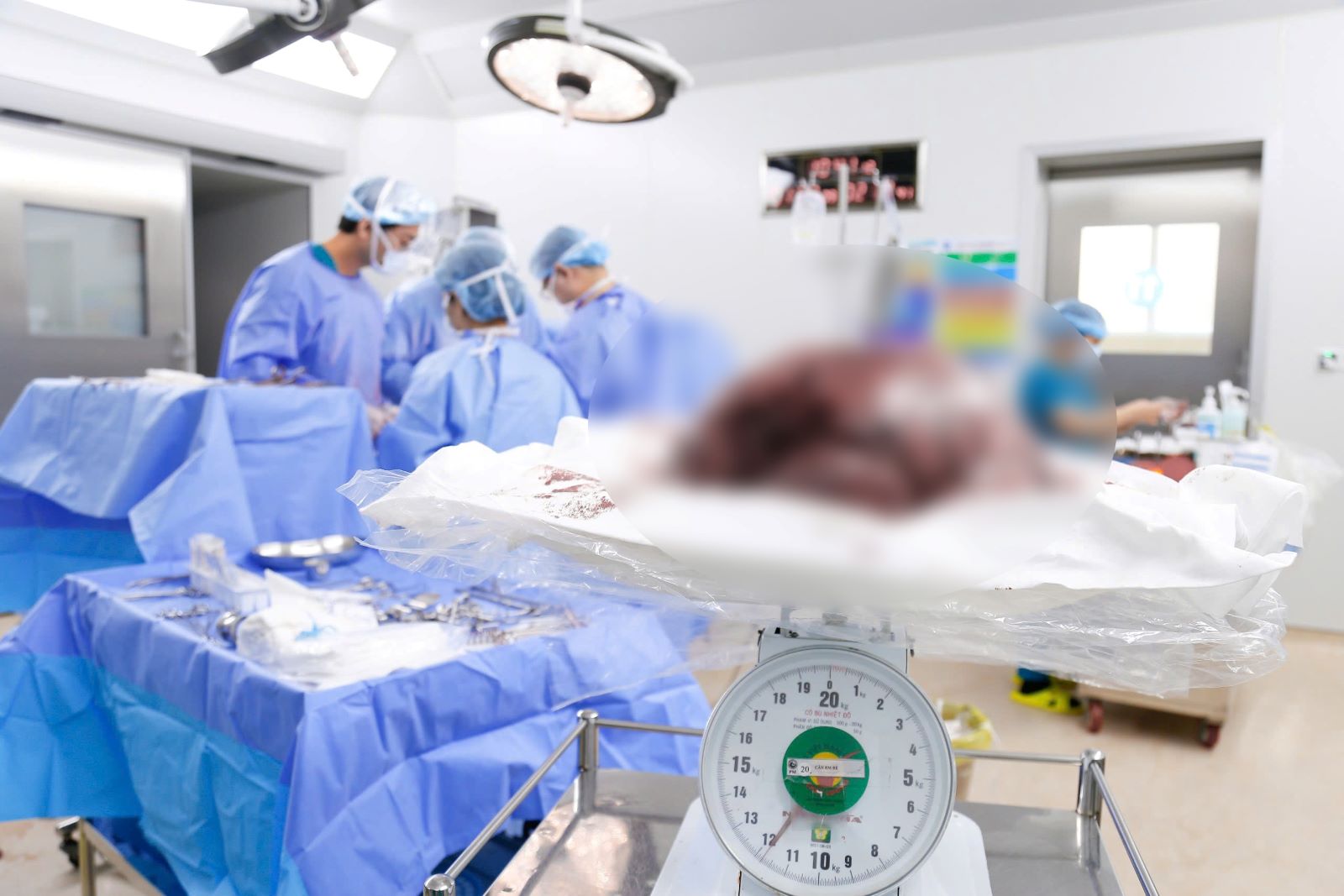
On March 25, Tu Du Hospital said that the unit had just successfully performed surgery, removing a very large uterine fibroid tumor weighing nearly 12kg for a 25-year-old female patient.
This is a complex pathological case when the patient not only carries a giant uterine fibroid tumor (equivalent to a 36-38 week pregnant twin) but is also accompanied by a femoral venous thrombosis, causing a near-complete stenosis of the lumen. This condition increases the risk of pulmonary embolism and cardiovascular events before, during and after surgery at a high to very high level.
Previously, the hospital had inter-hospital consultations many times with the Cardiology Department of Cho Ray Hospital, in order to comprehensively assess and develop an optimal treatment strategy. Patients were intervened with lower venous catheterization before surgery, helping to significantly reduce the risk of embolism.
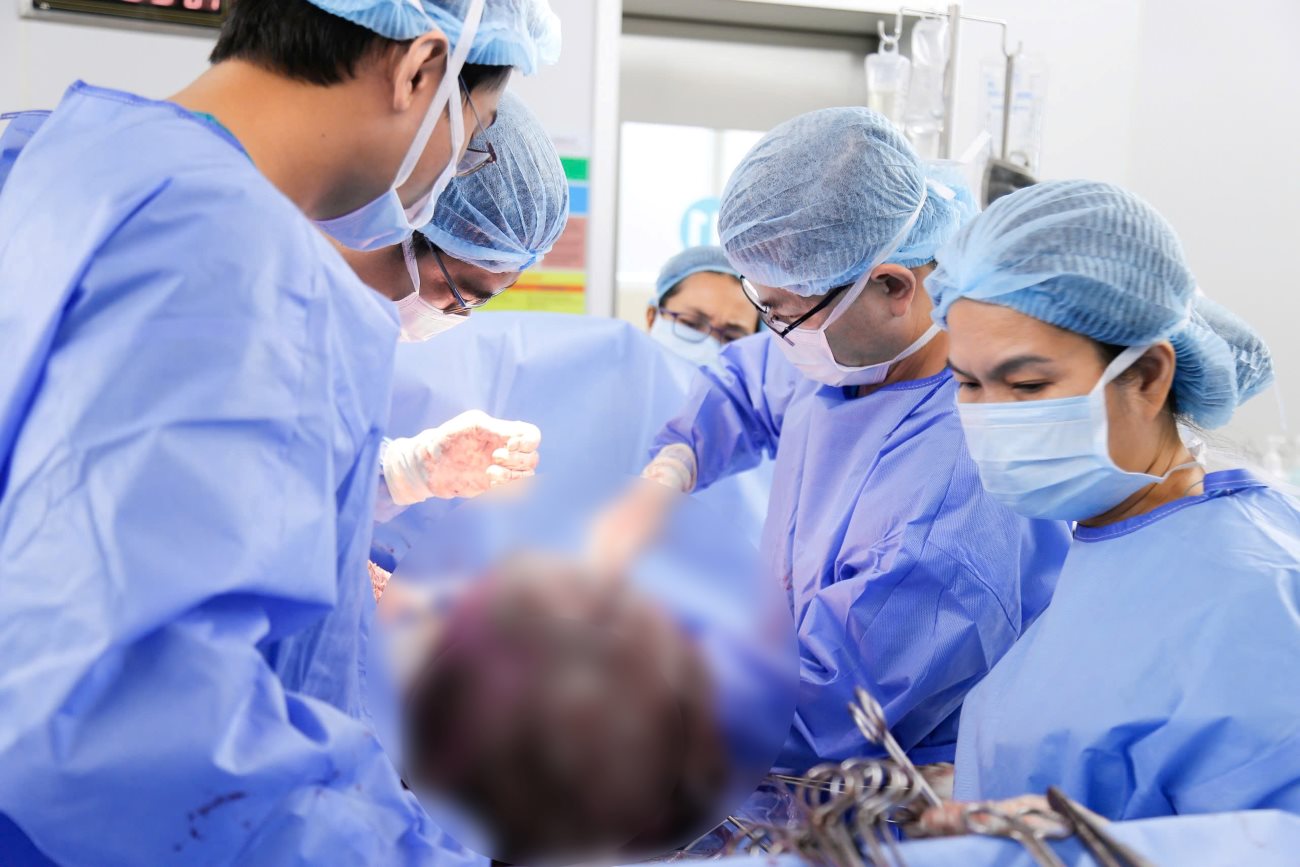
During the surgery on March 24, doctors recorded a large tumor, sticking tightly to many organs in the abdominal cavity. The tumor-nourishing blood vessel system proliferated strongly, with blood vessels up to 7mm in diameter, accompanied by many complex adhesions, increasing the risk of bleeding and complications.
The surgical team chose a vertical surgical route to ensure maximum exposure of the surgical site, creating conditions for safe treatment of large tumors. The surgical process encountered many difficulties, mainly in the stasis of removing adhesions and controlling the proliferative blood vessel system.
Notably, in the process of removing a tumor with a complex proliferative blood vessel system, the surgical team proactively applied a hemostatic technique using a rectangular stitch. This technique helps to effectively control widespread bleeding points, especially in the cut area and large blood vessel nodules, thereby minimizing blood loss during surgery.
The total amount of blood lost during surgery was about 500ml. The tumor was completely removed, without causing damage to adjacent organs. In particular, the patient's uterus was preserved, which is important for the patient who is still young and has not completed the reproductive plan.
By the afternoon of March 25, after 1 day of surgery, the patient could sit up, walk, and eat almost normally. The surgical wound was dry, without fever. The patient continued to receive anticoagulants and antibiotics.