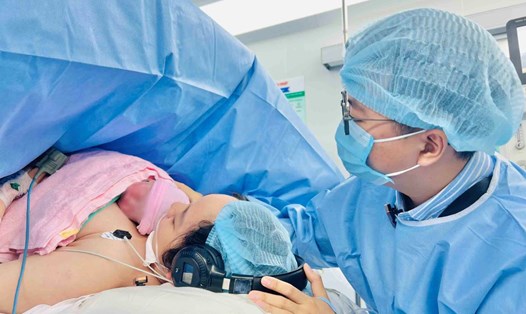
On the afternoon of October 2, information from Tu Du Hospital said that the unit had just coordinated with Children's Hospital 1 to successfully perform a cesarean section for Ms. H. The baby boy was born healthy, weighing 3kg, crying loudly, with rosy skin and mucous membranes, stable breathing and heart rate. The surgery was performed on September 26.
The baby was transferred to Children's Hospital 1 for further monitoring and treatment. After 5 days of post-surgery, on the morning of October 2, Ms. H was discharged from the hospital.
Previously, Ms. H's first trimester screening test had good results. At 22 weeks of pregnancy, an ultrasound examination revealed that the baby had a severe congenital heart defect and was transferred to Tu Du Hospital.
Here, prenatal ultrasound examination revealed that the fetus had severe pulmonary valve stenosis and severe tricuspid regurgitation grade 4/4. Doctors from Tu Du Hospital in collaboration with Children's Hospital 1 concluded that this was a case of no pulmonary valve opening - closed interventricular septum. This is a severe form of congenital heart disease requiring multiple surgical interventions.
At 25 weeks of pregnancy, the fetal heart rate worsened, with more severe right ventricular hypoplasia. Two weeks later, the situation worsened even more. Doctors decided to perform fetal valvuloplasty.
On July 19, the medical team from Tu Du Hospital and Children's Hospital 1 were ready to perform transuterine surgery to dilate the heart valve for Ms. H. After ultrasound intervention, the fetal heart was checked again and the flow through the pulmonary valve was good, with no pericardial effusion.
Ms. H's pregnancy progressed steadily. The baby's growth in length and weight were within normal limits. Ms. H continued to go to work every day until the baby was over 38 weeks old, when the obstetricians decided to terminate the pregnancy.
From January 2024 to present, Tu Du Hospital has performed fetal interventional cardiology to save the lives of 4 babies with severe congenital heart defects. These babies were all born healthy. After birth, the children developed physically and mentally well.
Successful fetal interventional cardiac catheterization surgery provides the last chance to save the life of a child with severe congenital heart disease.