On March 6, information from Can Tho Central General Hospital, doctors successfully performed endovascular intervention, promptly saving a case of severe bleeding due to invasive pharyngeal cancer in the internal carotid artery.
Female patient T.T. N. (48 years old, Can Tho City) was transferred to the hospital at 9:25 am on March 3 in a state of heavy bleeding from the nose and mouth, the patient was given initial hemostasis treatment at the previous level.
Through medical history, it was learned that the patient had a history of nasopharyngeal cancer and was undergoing chemotherapy. Immediately after being admitted to the hospital, the patient continued to vomit fresh red blood in large quantities accompanied by shortness of breath, low blood pressure with critical condition. The emergency team quickly performed intensive resuscitation, emergency blood transfusion, and at the same time performed a computed tomography (CT scan) with contrast agent injections to survey the nasopharyngeal area.
CT scan results recorded blockage damage in the area occupying the right lateral pharyngeal mucosal cavity, invasive of the inner carotid artery correspondingly, signs of fluorescence drug drain into the adjacent pharyngeal area and the pseudoaneurysm of the carotid artery in the lower base of the skull.
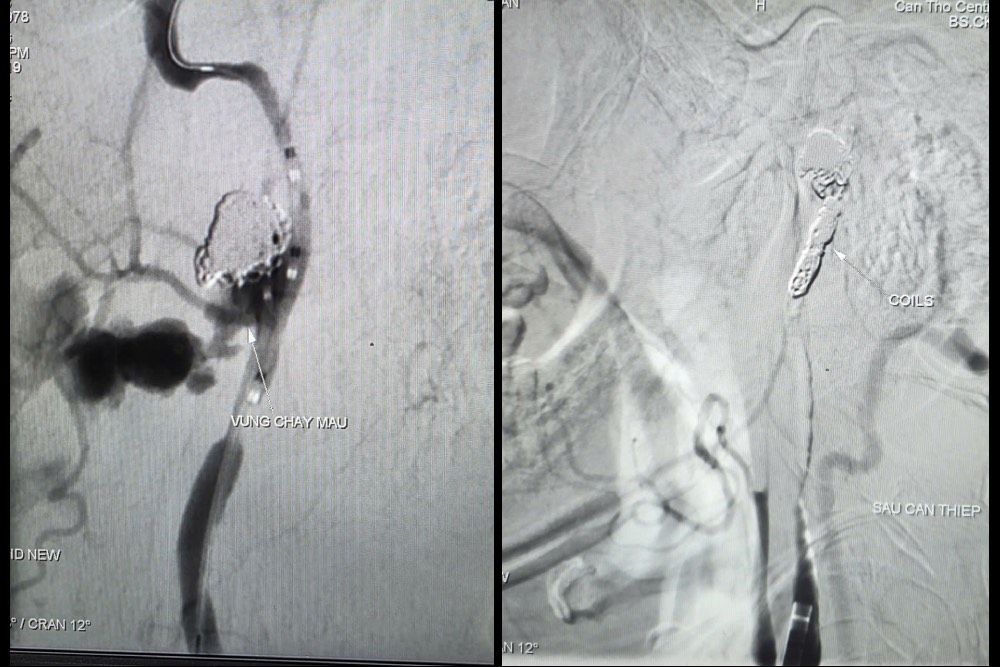
Faced with a critical situation, doctors decided to perform a scan and under-vascular hemostatic intervention (DSA). The results recorded a placental aneurysm of the inner right carotid artery in the neck, under the skull base, size 4.2 x 4.8 mm, the neck of the sac was swollen and bleeding.
Doctors blocked the flow to control the amount of blood flowing out of the aneurysm and continued to insert a selective microtubular catheter (super small catheter) to the location of the aneurysm and proceeded to release 09 metal coils to completely block the pseudoaneurysm and the right internal carotid artery, in order to thoroughly control the source of bleeding. An examination from the left internal carotid artery showed that there was circulatory flow of the right hemisphere feeding system through the anterior catheter artery, ensuring cerebral irrigation after intervention.
The completion time of intervention is 90 minutes.
On March 6, the patient was awake, had good contact, pink mucous membranes, no weakness or limb paralysis, and his health recovered positively.
According to BS.CKII. Nguyen Cong Dinh - Head of Oncology Department, Can Tho Central General Hospital, nasopharyngeal cancer is one of the cancers in the head and neck area with a very high level of local invasion due to the special anatomical characteristics of the nasopharynx. When the tumor progresses, the risk of direct spreading to adjacent tissues and penetrating vital structures is very high.
Endovascular intervention is considered a highly effective treatment, fast implementation time, and minimally invasive compared to open surgery. This technique allows access to lesions through the lumen, limits injury to healthy tissues, and shortens recovery time.
In recent years, the rate of endovascular intervention applications in the treatment of head, face, and neck tumors has been increasing, especially in cases of acute bleeding. The development of the digital background scanning (DSA) system, along with microtubules and new generation vascular nodules such as coils, biodegradable glue or nodules, has opened up opportunities for treatment for many patients.










