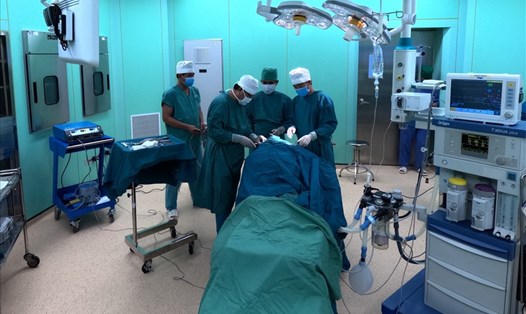
On January 8, 2025, the Department of Anesthesia and Resuscitation - Duc Giang General Hospital received pregnant woman L.T.N.T (23 years old, in Chuong My, Hanoi) from Viet Duc Friendship Hospital in critical condition. The patient was diagnosed with hospital pneumonia, traumatic brain injury ( subarachnoid hemorrhage, subaryongia subaring of the right frontal stripe), 26 weeks pregnant, and had an open tracheal chart.
When admitted to the hospital, the patient was in a coma, Glasgow had 7 points, all four limbs were stiff, and increased muscle tone. The CT results of the skull showed that the subary tract fluid was 9.5mm thick, suspected to be damage to the axons. Obstetrics and Gynecology face the risk of miscarriage, placental or slow-growing fetuses in the uterus at any time.
Dr. Le Nguyen An - Head of the Anesthesia and Resuscitation Department shared: "The biggest challenge is to ensure the health of both mother and fetus, while maintaining a gestational age of more than 30 weeks to increase the risk of survival and healthy development for the baby".
The medical team at Duc Giang General Hospital has coordinated with many specialties to develop an optimal treatment regimen. Caring for a coma patient with open airflow requires close monitoring to limit infection, malnutrition, acute alopecia and fetal ulcers and the risk of fetal failure.
The patient was treated with antibiotics for 10 days, actively cared for the lungs, closely monitored the fetal condition, had a fetal heart rate measured twice a day, and had a weekly ultrasound. In addition, the nutritional regimen is also constantly adjusted to ensure the health of both mother and baby.
After 70 days of treatment, the patient's condition improved significantly. tri tue giac quan improve from Glasgow 7 to 15 points, self-breathing through the airways, taking oxygen, and the fetus developing normally.
At 3:00 a.m. on March 15, the patient showed signs of early labor and rupture of the water source. The mother was consulted and immediately had a cesarean section. A 2,000-gram baby boy was born healthy, crying loudly, with rosy skin and good reflexes. The baby was given skin to the mother right after birth.
3 days after surgery, the mother was alert, ate naturally, had stable signs of neuropathy and had her tracheal opening removed. By the morning of March 20, the baby had been breastfed for the first time with the support of a nurse.
Tomorrow morning, March 21, 2025, the mother and child discharged from the hospital to end the miraculous journey of a mother through death's door to welcome her child to birth safely.