Elderly care workers are mainly relatives.
Mrs. Pham Thi Loan (name changed), 90 years old, in Son Tay town, Hanoi, had an accident and broke her thigh bone, and has been immobile for 8 years now. She has to rely on relatives to help her with all her eating and personal activities. Mrs. Loan's family had to assign a person to look after and care for her. "Taking care of the elderly is not hard but requires meticulousness, care, and psychology, from eating, bathing, going to the toilet... because the elderly are easily emotional and easily upset," said Mrs. Nguyen Thi Dung (name changed), 60 years old, a relative of Mrs. Loan, and this is just one of thousands of families with elderly people who need care.
Dr. Nguyen Trung Anh - Director of the Central Geriatric Hospital - said: "The ability to provide medical services for the elderly is currently very limited, from the lack of medical facilities such as hospitals, medical centers, health stations... and especially the lack of human resources to care for the elderly: geriatric specialists, geriatric nurses, caregivers... Currently, it mainly relies on family members, while this human resource is decreasing."
In addition, the system of nursing homes and social protection centers is limited in both quantity and quality. Knowledge of geriatrics is also lacking. Therefore, strengthening expertise as well as facilities and human resources in the treatment and care of the elderly is an urgent need and needs attention.
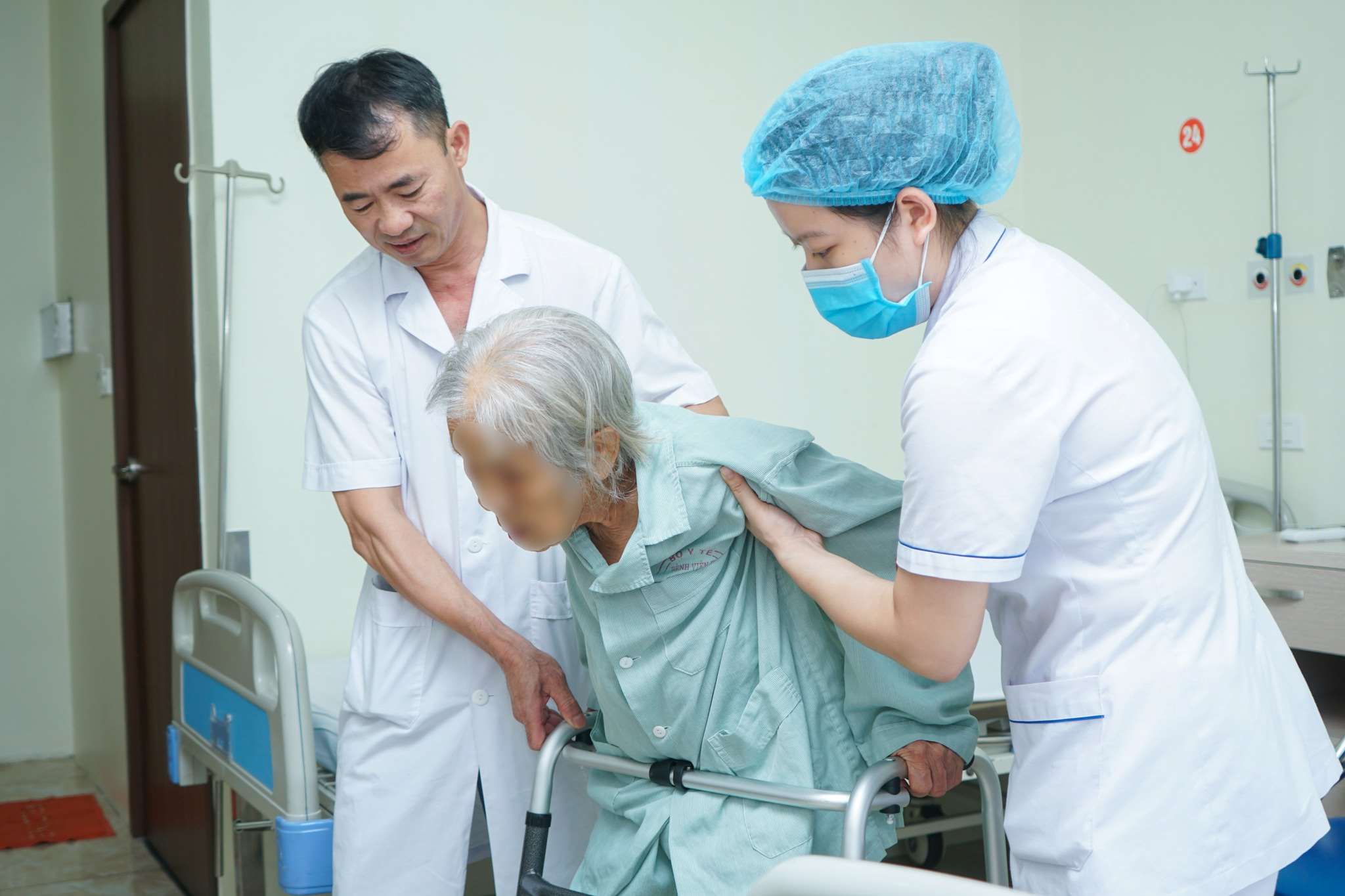
The entire Central line has only one geriatric hospital.
At the central level, there is only one geriatric hospital; provincial, district and primary health care levels nationwide have not yet invested in and focused on building a system including human resources, material resources and financial resources for elderly health care. In the provinces nationwide, only provincial hospitals and above have geriatric departments. The entire southern region does not have a single geriatric hospital.
This is a cause for concern as people’s life expectancy is increasing and the disease trend is shifting from infectious diseases to chronic diseases. Furthermore, at the commune level, there are only people who provide general primary health check-ups, there are no doctors specifically for geriatrics, and some health stations do not have doctors.
For example, in Hanoi, according to Associate Professor, Dr. Ho Thi Kim Thanh - Head of the Department of Family Medicine - Hanoi Medical University, the capital has about 250,000 people aged 75 and over, who need the most social, medical and care support. "It is estimated that the capital alone needs at least 10 hospitals, geriatric departments, and specialized geriatric care centers to serve the elderly," said Associate Professor, Dr. Ho Thi Kim Thanh.
Vietnam does not have a human resource system for elderly care. For example, nurses at the Central Geriatric Hospital must also work as caregivers - a huge pressure and they cannot fulfill this role.
Patients’ families often have to hire outside caregivers, which is both expensive and unsafe because they are not qualified or trained. They bring buckets, basins, and many other tools into the hospital, making the hospital space messy.
Medical costs and the burden of care for the elderly are 7-10 times higher than for young people. The elderly use up to 50% of all drugs. The increasing trend of deaths in medical facilities also increases medical costs. However, according to Associate Professor, Dr. Nguyen Trung Anh, these costs will be reduced if there are reasonable approaches.
Vietnam has officially entered the population aging phase since 2011 and is one of the countries with the fastest population aging rate in the world. It is forecasted that the number of elderly people in Vietnam will increase to 16.8 million by 2039 and reach 25.2 million by 2069.
Experts believe that it is necessary to soon have a strategy for care, monitoring and treatment for the elderly to become a complete system. That is, the family medicine system must form a principle of understanding the elderly, monitoring and caring for them in households and residential areas. From the initial formation, the grassroots health care lines must also build treatment facilities for the elderly, in particular, the areas should have specialized medical facilities, nursing and rehabilitation systems for the elderly.
The reason is that after treatment of diseases or complications, the elderly need care in nursing and rehabilitation.











